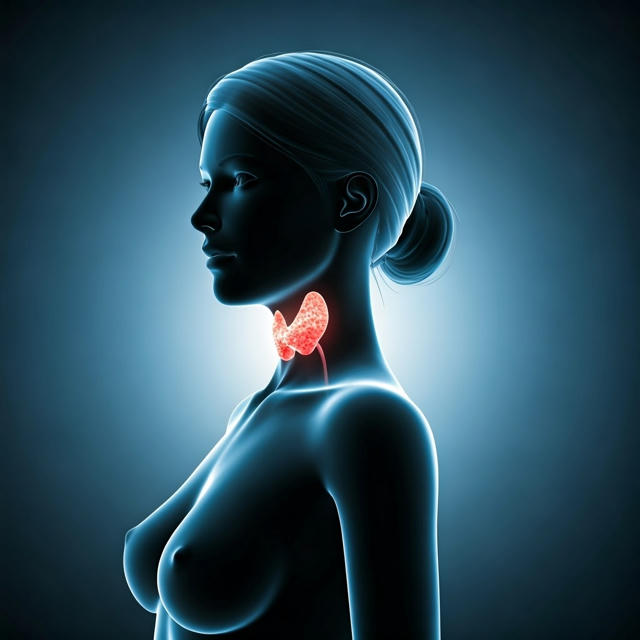
Understanding Your Thyroid Gland and Why Recovery Takes Time
The thyroid gland sits at the base of the neck and produces hormones that regulate your metabolism, energy levels, heart rate, and temperature. Removing part or all of it, whether due to cancer, goiter, hyperthyroidism, or suspicious nodules, disrupts those functions and disturbs the sensitive anatomy surrounding it. The gland sits near important nerves and the parathyroid glands, which is why recovery involves watching for specific complications and adjusting to hormonal changes. The closer you understand what the body is going through, the easier it is to follow your care instructions and recognize warning signs.
The Recovery Period: A Week-by-Week Breakdown
Recovery doesn’t happen all at once. It unfolds in layers, and knowing what each stage looks like helps you manage your expectations and energy.
Week 1: Rest and Wound Care
The first week is the most uncomfortable. You’ll likely spend the first day or two in the hospital, though many patients go home the same day for minimally invasive procedures. Expect fatigue, neck stiffness, and swelling around the incision. Most patients can eat soft foods and walk around the house, but lifting, straining, and intense activity are off-limits.
Keep the incision clean and dry as instructed
Sleep with your head slightly elevated to reduce swelling
Take prescribed pain medication on schedule, don’t wait for pain to spike
Avoid driving, especially while on narcotic pain relievers
Weeks 2–3: Gradual Return to Normal Activity
By the second week, most people feel noticeably better. Swelling begins to decrease, energy returns, and many patients return to desk jobs or light work. You may still feel some tightness in your neck when you turn your head, which is normal. Walking is encouraged; strenuous exercise is not.
Weeks 4–6: Getting Back to Full Strength
Physical restrictions lift significantly during this window. Most people can resume exercise, driving long distances, and more demanding work by week four or five. Your endocrinologist or surgeon will likely order blood work around this time to check your thyroid hormone levels and make any necessary medication adjustments.
Beyond Six Weeks
By weeks six to eight, most people feel like themselves again, sometimes better, since the underlying thyroid condition has been treated. The scar continues to fade over the following months, and hormone levels stabilize with proper medication management.
Managing a Sore Throat After Surgery
A sore throat is one of the most common complaints in the days following thyroid surgery, and it’s not caused by the neck incision alone. The breathing tube placed during general anesthesia irritates the throat lining, leading to rawness, scratchiness, and discomfort when swallowing. For most patients, this resolves within three to five days.
Sipping cool water, eating soft foods like yogurt or scrambled eggs, and using throat lozenges can all help. Gargling warm salt water is another simple remedy. If your sore throat gets significantly worse after day three, or if you have trouble swallowing liquids, reach out to your care team.
Dealing With a Hoarse Voice After Thyroidectomy
A hoarse voice after thyroid surgery is common and, in most cases, temporary. The recurrent laryngeal nerve, which controls vocal cord movement, runs directly behind the thyroid, and any irritation or swelling near it during surgery can affect voice quality. This doesn’t mean the nerve was damaged; often it’s simply inflamed.
Most hoarseness resolves within a few weeks as swelling subsides. Staying hydrated, resting your voice when possible, and avoiding whispering (which actually strains the cords more than normal speaking) can help the healing process. If hoarseness persists beyond six to eight weeks, your surgeon may refer you to a laryngologist to evaluate your vocal cords directly.
Recognizing Low Calcium Levels After Surgery
One of the more serious short-term complications of thyroidectomy is a drop in calcium, which can happen when the parathyroid glands are disturbed during surgery. These four tiny glands sit near the thyroid and regulate blood calcium levels. Even a temporary disruption can cause low calcium levels in the days after surgery.
Symptoms to watch for include:
Tingling or numbness in the fingers, toes, or around the mouth
Muscle cramping or twitching
A feeling of tightness across the chest
Anxiety or an unusual sense of unease
If you experience any of these, call your surgical team right away. Calcium supplements and vitamin D are typically prescribed as a precaution after total thyroidectomy, and most cases of low parathyroid function resolve on their own within weeks.
Thyroid Hormone Replacement Therapy: What You Need to Know
If your entire thyroid was removed, thyroid hormone replacement therapy is essential. Without it, your body cannot regulate metabolism, temperature, or energy. The most common medication is levothyroxine (Synthroid), a synthetic version of the hormone your thyroid used to produce.
Getting the dose right takes time. Your surgeon or endocrinologist will start you on a dose based on your weight and health history, then fine-tune it based on blood work at six weeks, three months, and beyond. During this adjustment period, you may notice symptoms of being over- or under-medicated: fatigue, weight changes, mood shifts, or heart palpitations. These are signals to check in with your doctor, not reasons to stop taking your medication.
If only part of your thyroid was removed, your remaining tissue may produce enough hormone on its own, though this varies and requires monitoring.
Recovery Time After Robotic Thyroid Surgery
Robotic thyroid surgery is an increasingly popular minimally invasive option that allows surgeons to remove the thyroid through small incisions made in less visible locations, typically the armpit or behind the ear, rather than the neck. Because there is no neck incision, many patients experience less visible scarring and sometimes find the cosmetic outcome more acceptable.
The recovery time for robotic thyroid surgery is generally similar to traditional open surgery, though some patients report less neck stiffness in the early weeks. The same risks, including temporary hoarseness and calcium fluctuations, still apply, since the internal anatomy involved is identical. Dr. Suh, a specialist in robotic and minimally invasive thyroid surgery, has noted that although the approach to the gland varies, patient recovery milestones tend to follow a similar week-by-week pattern. Most patients return to work within one to two weeks and feel fully recovered by week six.
When to Contact Your Surgeon During Recovery
Knowing when to call is just as important as knowing what’s normal. Contact your surgeon promptly if you experience:
Rapidly expanding swelling or firmness at the incision site
Difficulty breathing or swallowing that worsens suddenly
Fever above 101°F (38.3°C)
Tingling, numbness, or muscle cramping (possible low calcium)
Significant hoarseness that appears or worsens after the first week
Heavy bleeding or discharge from the incision
Most thyroid surgery recoveries go smoothly, but early communication with your care team can make the difference between a minor issue and a serious complication. Trust your instincts – if something feels off, it’s always worth a call.
Making Your Decision
Choosing between robotic and traditional thyroid surgery shouldn’t be based solely on scar avoidance. Consider these factors:
- Medical factors: What does your disease require? Some conditions simply aren’t suitable for remote-access approaches.
- Surgeon expertise: Has your surgeon performed hundreds of the specific procedure you’re considering? Experience matters enormously in thyroid surgery.
- Personal priorities: How important is avoiding a neck scar relative to other factors like cost, operative time, and recovery?
- Realistic expectations: Understand that robotic approaches still create scars – just in different locations – and that these alternative incisions carry their own healing considerations.
The best choice is the one that addresses your medical needs effectively while aligning with your personal circumstances. Have an honest conversation with your surgeon about what matters most to you, and trust their guidance about which approach gives you the best overall outcome. Remember that thousands of patients achieve excellent results with traditional surgery every year, and the neck scar from modern techniques is typically far less noticeable than many people fear.
Conclusion
Recovering from thyroid surgery, whether you had a partial removal or lost your whole thyroid due to thyroid cancer or another condition, is a process that rewards patience and attention. In the early days, staying on top of pain management matters more than most patients expect; taking narcotic pain medications before discomfort peaks, rather than after, makes a real difference in how comfortable those first nights feel. As the weeks progress, small milestones add up: swallowing becomes easier as difficulty swallowing fades, your energy returns as blood flow to the healing tissue normalizes, and your incision gradually becomes something you barely notice. Taking your levothyroxine on an empty stomach each morning becomes second nature, and routine blood tests shift from anxiety-inducing appointments to simple check-ins.
The road back to yourself is shorter than it seems at the start.

About the Author
Dr. Hyunsuk Suh, MD
Director of Operations | Authorized Vampire Facelift® Professional | Injectable Expert & Certified Galderma Trainer
Empowering
Women’s Health

By Dr. Hyunsuk Suh, MD
February 19, 2026